Introduction
The rise in prescriptions for Ozempic, a medication traditionally used to manage type 2 diabetes, signals a significant change in how we approach obesity in modern healthcare. We understand that many individuals struggle with weight management, and Ozempic offers a promising solution by mimicking hormones that regulate appetite and promote weight loss. In a society that is increasingly open to medical interventions, this medication could be a beacon of hope for those facing these challenges.
However, as its popularity continues to grow, we must consider some important questions:
- What does this mean for patients seeking effective solutions?
- Is the weight loss achieved through this treatment sustainable in the long run?
- What are the ethical implications of prescribing Ozempic for weight management?
These are crucial considerations for both patients and healthcare providers.
As we navigate this complex landscape of obesity treatment, it’s essential to approach these questions with empathy and understanding. You’re not alone in this journey, and together, we can explore the best paths forward.
Understand the Medical Rationale for Prescribing Ozempic
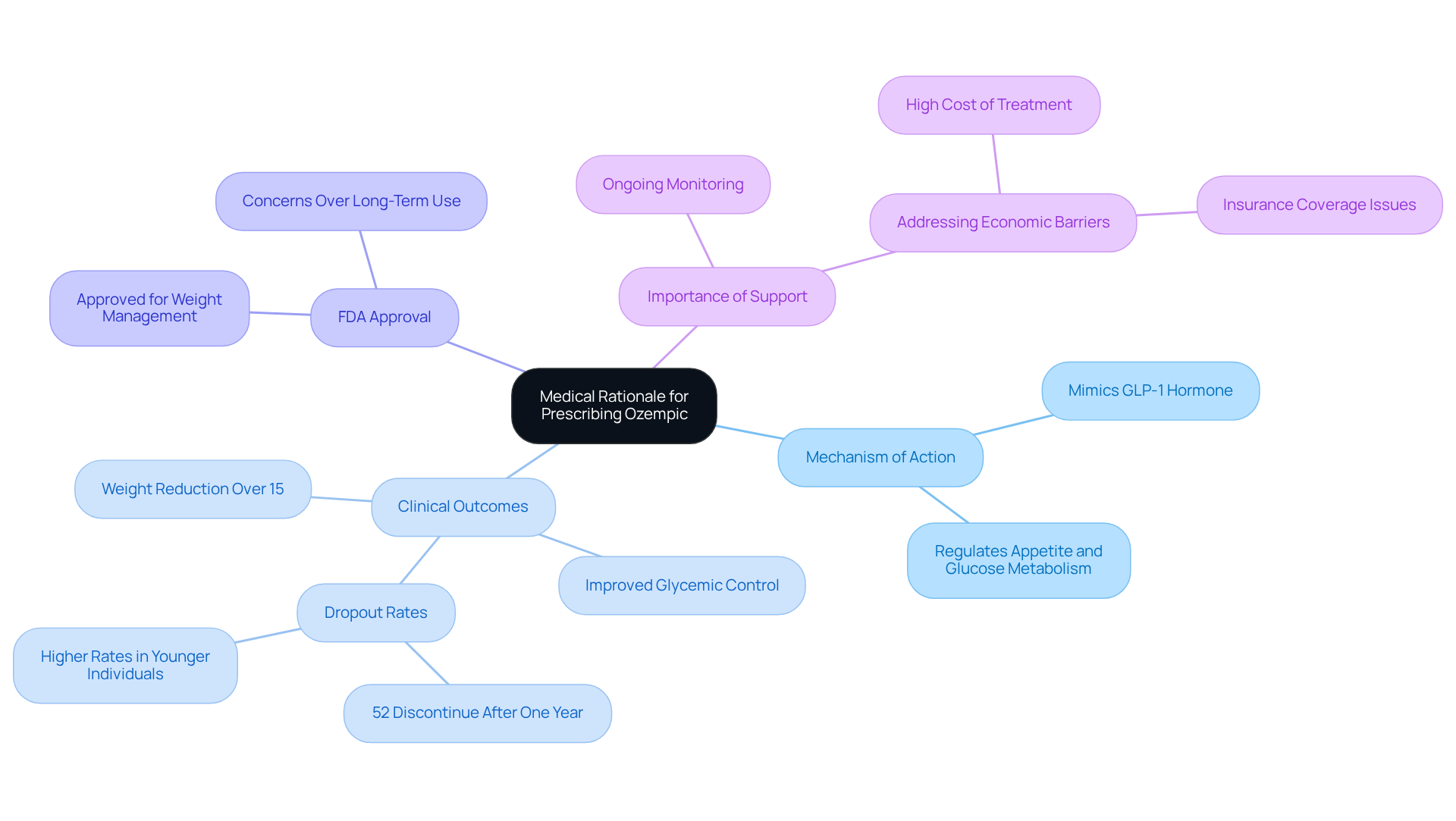
Semaglutide is a medication that many people turn to for managing type 2 diabetes, and it does so by mimicking the GLP-1 hormone, which plays a vital role in regulating appetite and glucose metabolism. We understand that managing weight can be a significant challenge, and semaglutide helps by increasing feelings of fullness and reducing food intake. This can lead to substantial weight loss, making it a hopeful option for those facing obesity.
Clinical studies show that patients using semaglutide can achieve weight reductions of over 15% within a year. This is an important outcome, especially as healthcare increasingly recognizes obesity as a chronic condition that needs more than just lifestyle changes. The FDA’s approval of semaglutide for weight management raises important questions about whether doctors are prescribing Ozempic for weight loss, underscoring its potential to change the way we approach obesity treatment and marking a shift in how healthcare professionals support individuals in their weight loss journeys.
As Dr. Maria Daniela Hurtado Andrade points out, while semaglutide is effective, it’s crucial to consider why doctors are prescribing Ozempic for weight loss long-term for lasting results. This highlights the importance of ongoing support and monitoring for patients, ensuring they can maximize the benefits of this treatment. Remember, you’re not alone in this journey; with the right support, achieving your health goals is within reach.
Examine Societal Influences on Ozempic’s Popularity
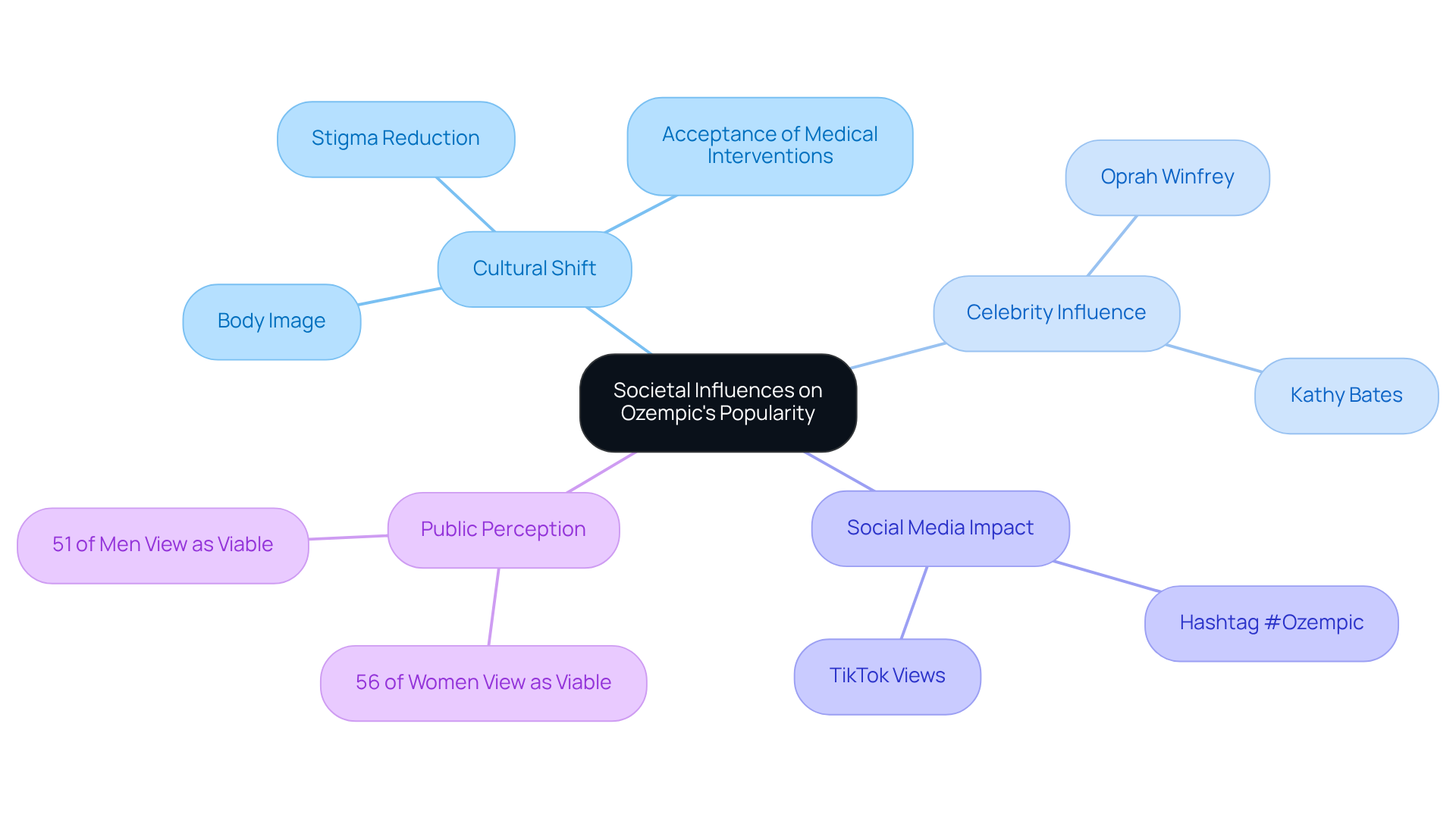
The rise in popularity of this medication as a way to reduce body mass is closely tied to evolving societal views on obesity and health. We understand that many people struggle with body image and weight, and in recent years, there’s been a cultural shift that frames slimming treatments as not just acceptable, but desirable. This is especially true among celebrities and influencers who openly share their journeys with such medications. Social media platforms play a vital role in amplifying these narratives, often glamorizing quick fixes for body mass reduction and fostering the belief that medications like Ozempic can provide a swift solution. This trend reflects a diminishing stigma around obesity, leading to greater acceptance of medical interventions for managing body mass.
Statistics show that about 56% of women and 51% of men familiar with these medications view them as viable options for reducing body mass. This growing acceptance is evident in the increasing number of prescriptions for this medication, as individuals actively seek effective solutions to combat obesity, leading to discussions about how many are doctors prescribing ozempic for weight loss in a culture that increasingly values health and appearance. Notable figures like Oprah Winfrey and Kathy Bates have candidly discussed their experiences with slimming treatments, contributing to a broader conversation that normalizes their use.
Moreover, the impact of social media is significant. The hashtag #Ozempic has garnered millions of views on platforms like TikTok, showcasing personal fitness journeys and further driving demand. As public figures share their successes and challenges, they shape perceptions and inspire others to consider similar paths. This interplay between societal views and medical methods is crucial for understanding the current landscape of body mass management, highlighting the important role that cultural narratives play in the acceptance and use of slimming substances.
You’re not alone in this journey. Many are navigating similar paths, and it’s essential to approach these conversations with compassion and understanding.
Explore Ethical Concerns in Prescribing Ozempic
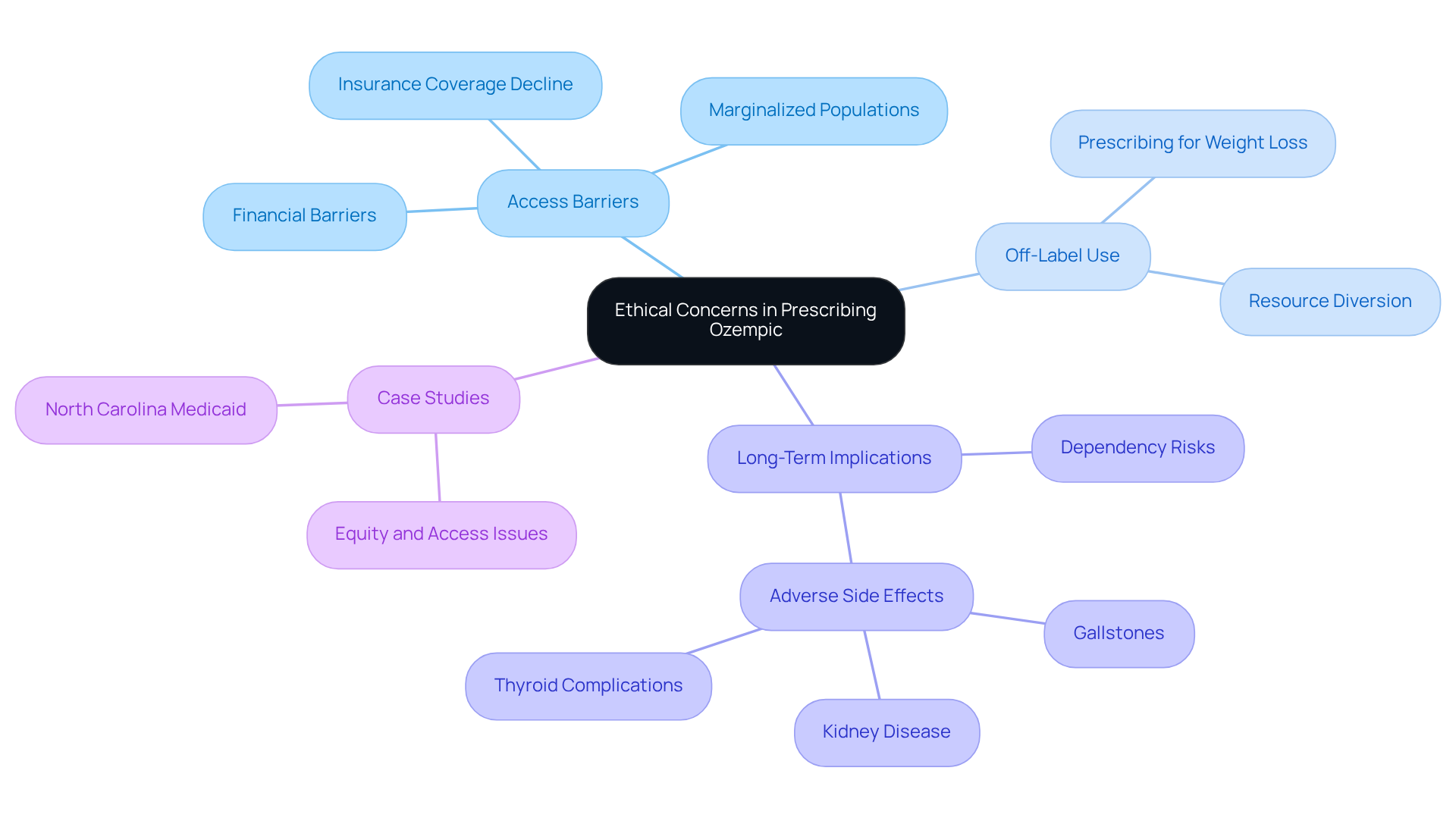
The important ethical concerns that arise from the prescription of medication, particularly regarding doctors prescribing ozempic for weight loss, deserve our attention. We understand that access to these drugs can be a significant barrier, especially for those who may not have the financial means. This often leaves marginalized populations without the treatment options they desperately need.
Moreover, the off-label use of these medications complicates the situation further. When we consider that many are doctors prescribing ozempic for weight loss, it raises questions about whether prescribing a diabetes treatment to individuals without diabetes is truly serving those who need it most. It’s crucial to consider the potential diversion of vital resources from patients who genuinely require them.
As we navigate these complex issues, we must also think about the long-term implications of using such treatments. There are risks of dependency and adverse side effects, including gallstones, kidney disease, and thyroid complications. In 2023, we saw a significant drop in the approval rate for insurance coverage of Ozempic, plummeting from 60% in 2022 to just 25%. This stark decline highlights the growing disparities in access to weight management treatments.
As healthcare providers confront these ethical dilemmas, it’s essential to prioritize patient well-being. We must ensure that our prescribing practices align with the principles of equity and justice in healthcare.
Consider the case studies that illustrate these disparities. In North Carolina, for instance, the removal of Medicaid coverage for GLP-1s has resulted in many patients regaining weight due to lack of access. Reports indicate that a significant number of individuals have struggled to maintain their weight loss after losing coverage. Experts emphasize that those with substantial medical needs should be prioritized for these treatments. Relying solely on pharmacological solutions could exacerbate existing health disparities.
Ultimately, addressing these ethical concerns is vital for creating a more equitable healthcare system. You’re not alone in this journey; together, we can advocate for a system that truly supports everyone.
Assess Long-Term Implications of Ozempic Use for Weight Loss
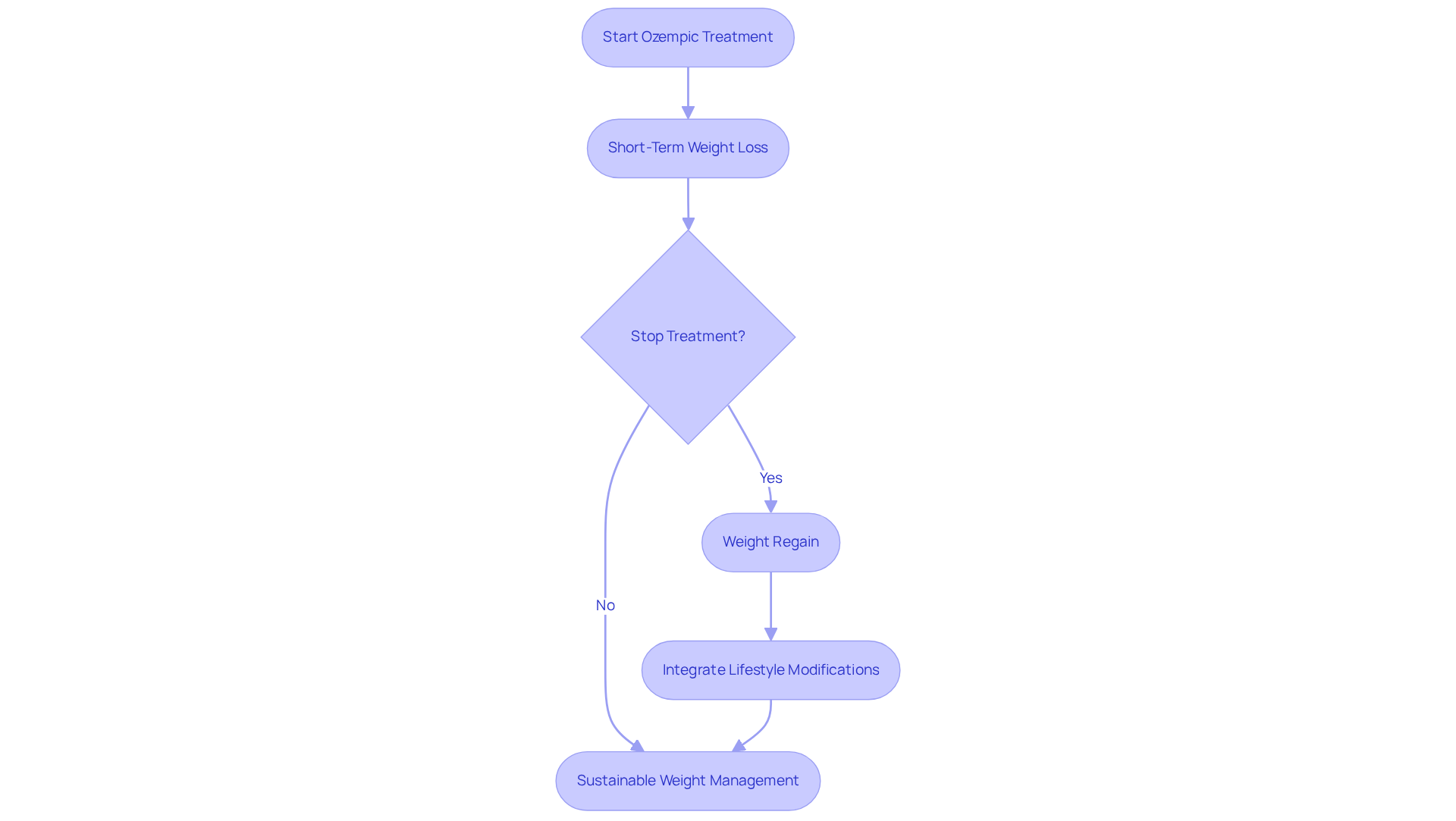
Ozempic has shown significant short-term weight loss advantages, but we understand that its long-term effects need careful evaluation. Many patients face the challenge of regaining weight after stopping treatment, which can be disheartening. Research indicates that a lot of individuals return to their pre-treatment size levels. In fact, studies reveal that participants who stopped semaglutide regained about 12% of their lost mass within a year. This raises important questions about how sustainable the reductions achieved through GLP-1 treatments like Ozempic really are.
In a 2021 trial, participants who discontinued semaglutide treatment after 20 weeks found themselves roughly 4% below their initial weight nearly a year later. This suggests that while some reduction may be retained, the majority is often regained. Furthermore, a 2023 study on tirzepatide showed that participants retained almost 10% of their weight loss a year after stopping treatment, but the long-term viability of such outcomes remains uncertain.
It’s also important to note that discontinuing Ozempic can lead to gastrointestinal side effects, which may impact a patient’s overall quality of life. Therefore, healthcare providers must emphasize the importance of integrating lifestyle modifications – like improved nutrition and regular exercise – alongside pharmacological treatments. At CT Medical Weight Loss & Beyond, we understand that this journey can be challenging. That’s why we offer customized nutrition plans tailored to individual needs, along with structured support through our 10 Point Touch System.
This comprehensive strategy is crucial in addressing the challenges of weight management and preventing the cycle of weight regain after stopping medication. We want to ensure that you not only achieve weight loss but also maintain your health and well-being over time. You’re not alone in this journey, and we’re here to support you every step of the way.
Conclusion
The rising trend of doctors prescribing Ozempic for weight loss marks a significant change in how we view obesity in the medical field. Originally intended for managing type 2 diabetes, this medication has caught attention for its ability to help with weight management by making people feel fuller and reducing their food intake. As healthcare professionals increasingly recognize obesity as a chronic condition that needs comprehensive treatment, Ozempic’s role has become more prominent.
We understand that many individuals struggle with weight management, and the medical rationale behind prescribing Ozempic is compelling. Clinical studies show its effectiveness in promoting substantial weight loss. Additionally, societal influences – like evolving perceptions of body image and the impact of social media – have led to a growing acceptance of this medication as a viable weight loss solution. However, it’s important to consider the ethical concerns surrounding access and the appropriateness of off-label use, which raise vital questions about equity in healthcare and the long-term implications of such treatments.
If you’re considering Ozempic, it’s crucial to have informed discussions with your healthcare provider about the benefits and risks associated with its use. We encourage you to adopt a holistic approach that includes lifestyle changes alongside pharmacological interventions, as this can enhance the sustainability of your weight loss outcomes. As the conversation around Ozempic continues to evolve, fostering awareness and understanding will be key to ensuring that everyone has equitable access to effective weight management solutions. Remember, you’re not alone in this journey, and support is available.
Frequently Asked Questions
What is semaglutide and how does it work for managing type 2 diabetes?
Semaglutide is a medication that mimics the GLP-1 hormone, which regulates appetite and glucose metabolism, thereby helping individuals manage type 2 diabetes.
How does semaglutide assist with weight management?
Semaglutide increases feelings of fullness and reduces food intake, which can lead to significant weight loss, making it a hopeful option for those facing obesity.
What kind of weight loss can patients expect from using semaglutide?
Clinical studies show that patients using semaglutide can achieve weight reductions of over 15% within a year.
Why is the FDA’s approval of semaglutide for weight management significant?
The FDA’s approval highlights the recognition of obesity as a chronic condition that requires more than just lifestyle changes and marks a potential shift in how healthcare professionals approach obesity treatment.
What should be considered when prescribing Ozempic for weight loss?
It is crucial to consider the need for ongoing support and monitoring for patients to maximize the benefits of semaglutide for long-term weight loss results.
How can patients ensure they achieve their health goals while using semaglutide?
Patients can achieve their health goals by seeking the right support and monitoring throughout their treatment journey with semaglutide.




