Introduction
Polycystic Ovary Syndrome (PCOS) is a complex hormonal disorder that affects many women, often leading to a range of health challenges, including infertility and metabolic issues. We understand that navigating this condition can feel overwhelming. Amidst these complexities, the potential impact of weight loss shines as a beacon of hope. Many wonder if shedding pounds could help alleviate their symptoms.
But the journey toward effective weight management is filled with questions and contradictions. Can losing weight truly transform the experience of living with PCOS, or is it just one piece of a larger puzzle? Exploring this connection reveals not only the importance of personalized strategies but also the profound implications for women seeking to regain control over their health.
You’re not alone in this journey. Many women have found that tailored approaches to weight management can lead to significant improvements in their symptoms. In addition, understanding your body and its unique needs can empower you to make informed choices. Remember, every step you take is a step toward better health.
Define Polycystic Ovary Syndrome (PCOS): Understanding the Condition
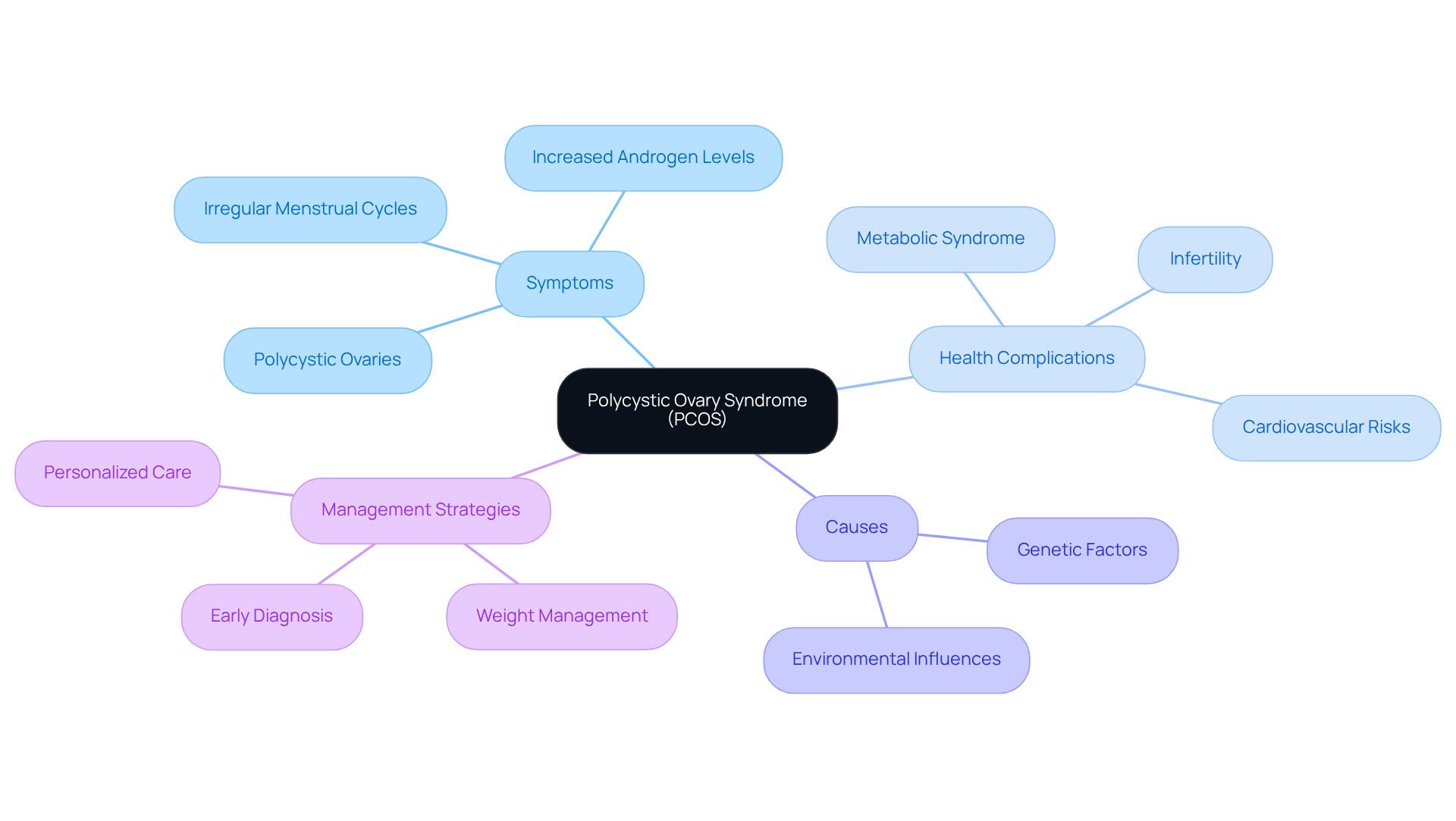
is a common hormonal condition that affects many women of reproductive age. It can lead to irregular menstrual cycles, increased androgen levels, and the presence of polycystic ovaries. We understand that dealing with PCOS can be overwhelming, as it’s linked to various health complications, including infertility, metabolic syndrome, and a heightened risk of type 2 diabetes. Recent studies show that PCOS isn’t just a reproductive issue; it’s a lifelong multisystem disorder that can significantly affect both cardiovascular and psychological health.
The exact cause of PCOS remains unclear, but it’s believed to arise from a complex mix of genetic factors and environmental influences. A key aspect of PCOS is its connection to weight gain, which can lead to obesity and raises the concern of if I lose weight will my PCOS go away, making it challenging for many individuals to manage their body size. In fact, research indicates that women with PCOS often face struggles with obesity and insulin resistance. This makes weight management crucial for improving overall health outcomes, particularly in relation to the question of if I lose weight will my PCOS go away.
Current guidelines emphasize the importance of early diagnosis and tailored treatment strategies. It’s now recognized that PCOS increases the risk of cardiovascular diseases, highlighting the need for preventive measures. These strategies should address not only the reproductive aspects of the condition but also its metabolic and psychological effects. As research continues to evolve, the focus on personalized care and innovative treatment options, such as lifestyle modifications, is becoming increasingly vital for those navigating the challenges of PCOS.
You’re not alone in this journey. With the right support and understanding, it’s possible to manage symptoms and improve your quality of life.
Explore the Connection Between PCOS and Weight Management
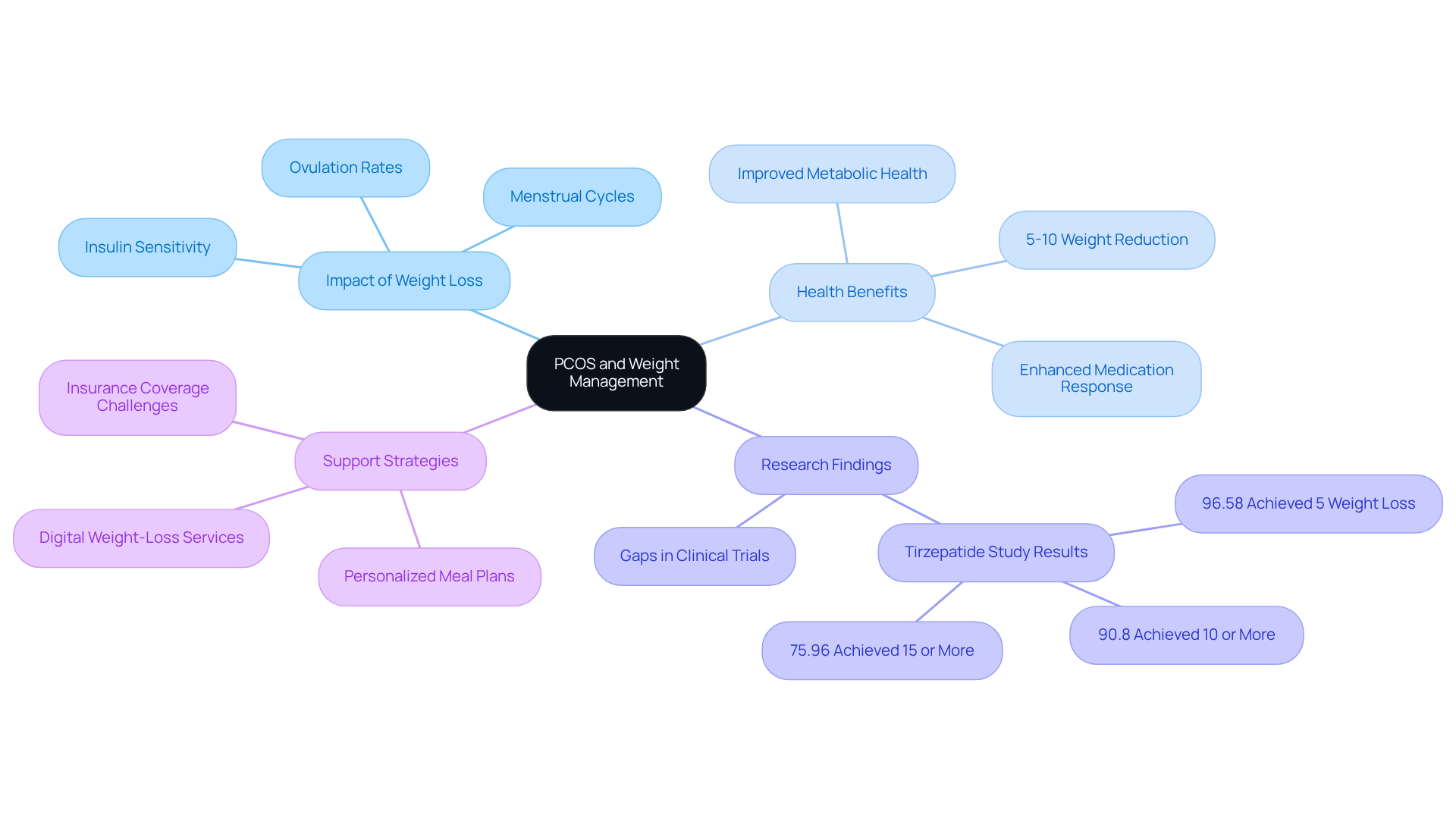
Research highlights a significant connection between polycystic ovary syndrome (PCOS) and the inquiry of weight management. Many individuals diagnosed with this condition are often concerned about whether if they lose weight will their PCOS go away, as they struggle with being overweight or obese. We understand that if I lose weight, will my PCOS go away, since weight gain can worsen insulin resistance, a common challenge in PCOS, leading to further and intensified symptoms.
A modest weight reduction of just 5-10%, which makes me wonder about its impact. This reduction is linked to better hormonal balance, more regular menstrual cycles, and increased ovulation rates. Managing body mass is crucial in effectively handling PCOS, which raises the question: what are the best strategies for weight loss?
At CT Medical Nutrition & Beyond, we’re here to support you with personalized plans and our 10 Point Touch System, ensuring you receive the guidance you need to achieve your goals. For example, a study involving women with PCOS who were prescribed lifestyle interventions showed that an impressive 96.58% of participants experienced at least a 5% loss in body mass. This demonstrates the effectiveness of thoughtful management strategies.
However, we recognize that there are still gaps in research, especially regarding medication options for PCOS. Additionally, many patients encounter hurdles with insurance coverage for these medications, which can limit access to effective treatment options.
Incorporating insights from experts like Dr. Stephanie Estes, who emphasizes the importance of lifestyle changes, can help clarify the complexities of managing PCOS through weight loss. Remember, you’re not alone in this journey, and we’re here to help you every step of the way.
Identify Effective Weight Loss Strategies for Managing PCOS
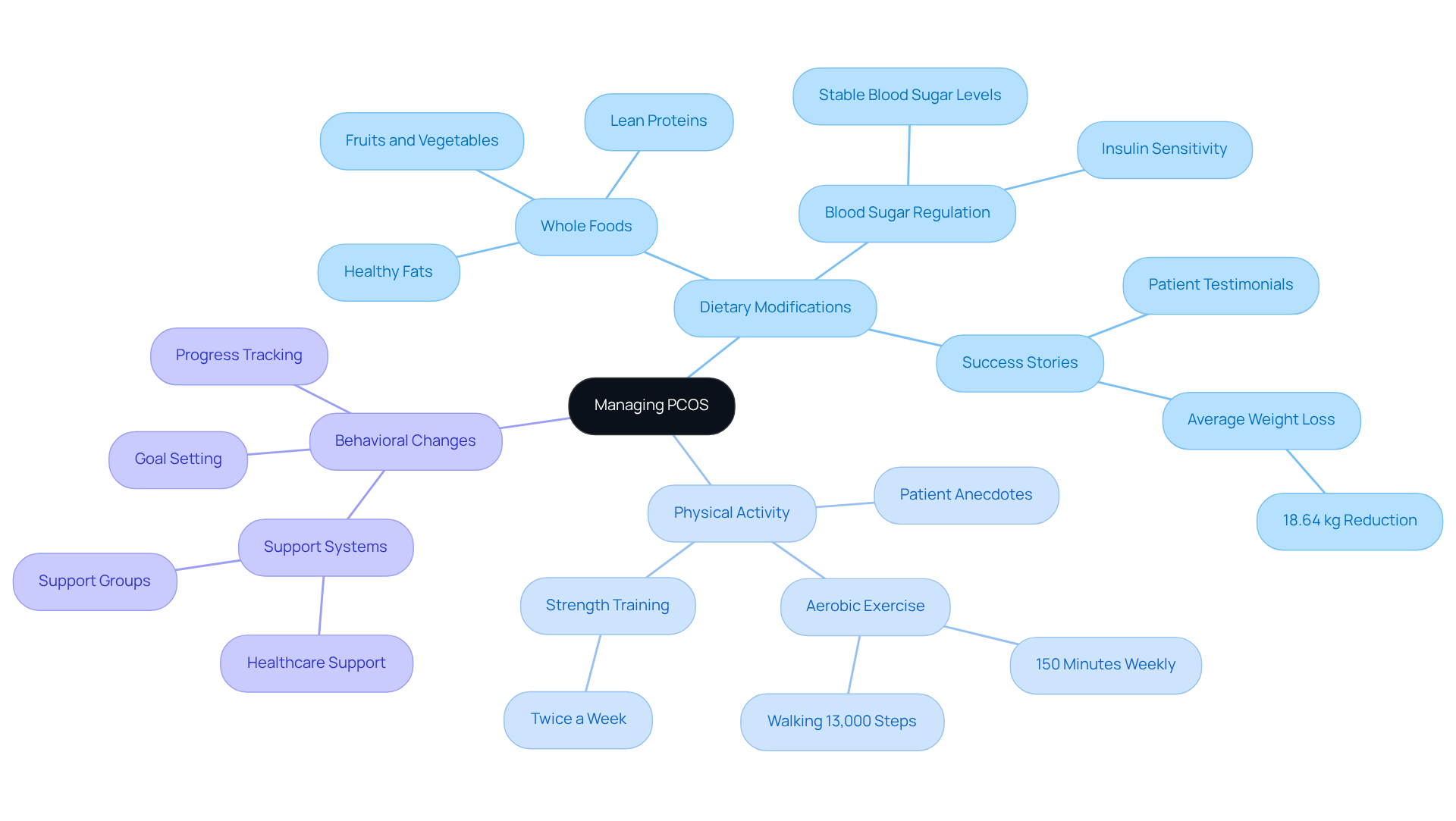
Managing Polycystic Ovary Syndrome (PCOS) can feel overwhelming, but support is available. At CT Medical Weight Loss & Beyond, we understand that a multifaceted approach is essential. This includes dietary modifications, physical activity, and behavioral changes tailored just for you.
Imagine having a program to promote healthy eating and stable blood sugar-crucial for women with PCOS. By emphasizing whole foods like fruits, vegetables, lean proteins, and healthy fats, you can play a vital role in regulating your blood sugar levels and enhancing insulin sensitivity. Many women have shared their success stories, reporting weight loss and symptom improvement through personalized plans. In fact, some have achieved an average reduction of 18.64 kg in studies focused on personalized interventions.
In addition to nutrition, consistent physical activity is key. Blending aerobic and strength training can enhance your weight management and metabolic health. Fitness experts recommend aiming for at least 150 minutes of moderate-intensity aerobic activity each week, along with strength training exercises twice a week. This combination not only helps in weight loss but also boosts your overall physical fitness and emotional well-being. Anecdotal evidence from our patients suggests that sticking to exercise routines, like walking 13,000 steps daily, can lead to significant reductions in body mass when paired with dietary changes.
Moreover, behavioral strategies can further enhance the effectiveness of these interventions. Setting attainable goals, tracking your progress, and seeking support from healthcare experts can greatly contribute to achieving and maintaining a reduction in body mass. Individuals who engage in counseling or work closely with dietitians at CT Medical Weight Management & Beyond often report greater success in their weight loss journeys. Our structured support, including the 10 Point Touch System and regular communication through weekly emails and monthly newsletters, ensures you receive ongoing guidance and motivation.
In some cases, medications like metformin, available through our advanced therapies, can be beneficial for those struggling to see results through lifestyle changes alone. These medications have shown promise in facilitating fat reduction and improving metabolic health, making them a valuable option for women with PCOS facing unique challenges in managing their body composition.
Ultimately, a comprehensive plan that integrates nutrition, physical activity, and behavioral changes-backed by the organized programs at CT Medical Weight Management & Beyond-can help answer the question of ‘if I lose weight will my PCOS go away’ by leading to successful body mass reduction and better control of PCOS symptoms. Remember, you’re not alone in this journey, and with the right support, you can achieve your health goals.
Emphasize the Need for Personalized Weight Loss Solutions in PCOS
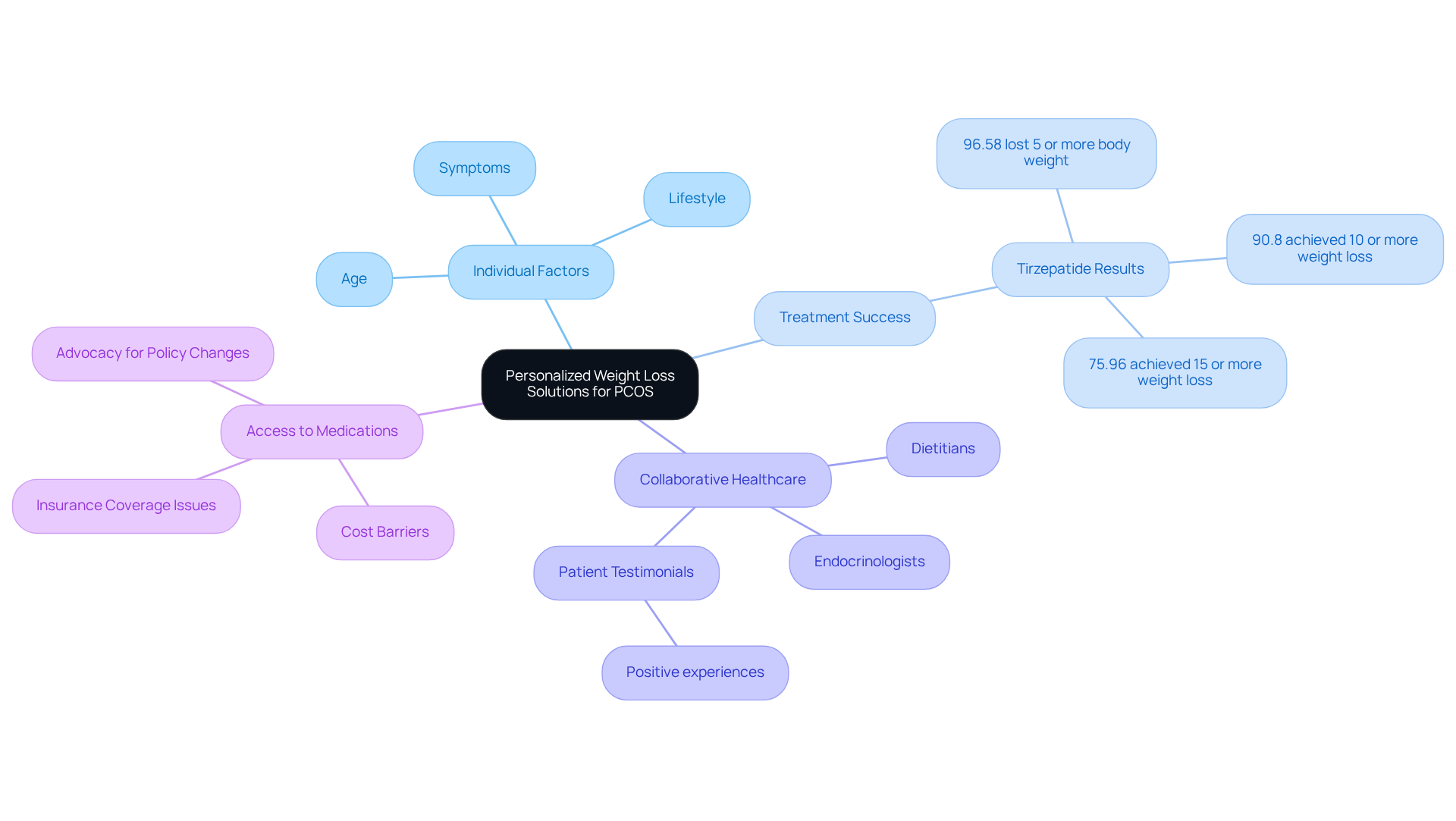
Polycystic ovary syndrome (PCOS) presents a unique set of challenges, and we understand that managing this condition can feel overwhelming. Each person’s journey with PCOS is different, influenced by factors like age, lifestyle, and specific symptoms. That’s why a one-size-fits-all approach often falls short.
At CT Medical Weight Loss & Beyond, we believe in creating plans that consider your personal dietary preferences, activity levels, and any existing health conditions. For instance, research indicates that an impressive weight loss occurs after just 10 months of treatment with tirzepatide, leading to the question, what are the best practices? This highlights the power of personalized strategies tailored to your needs.
Collaboration with healthcare professionals, including dietitians and endocrinologists, is crucial in developing a plan that addresses the specific hurdles you may face. As one satisfied patient shared, “Coming to CT was the best decision I’ve made in a long time. The staff is conscientious, knowledgeable, and very accommodating.” This collaborative approach not only boosts your chances of successfully managing your body mass but also fosters relationships that can enhance your overall health.
Moreover, treatment options, like those available at CT Medical, can vary, raising the question of what is most effective. Our team also offers tailored support to help you achieve your weight loss goals effectively.
However, we recognize that accessing these medications can be challenging due to high costs and insurance coverage issues. This underscores the importance of advocacy in this area. Remember, you’re not alone in this journey; we’re here to support you every step of the way.
Conclusion
Understanding the relationship between Polycystic Ovary Syndrome (PCOS) and weight management is crucial for improving health outcomes. We know that losing weight might not completely eliminate PCOS, but it can significantly alleviate symptoms, enhance insulin sensitivity, and promote overall well-being. This connection highlights the need for personalized approaches that cater to individual needs and challenges.
Even a modest weight loss of 5-10% can lead to substantial improvements in metabolic and reproductive health for those with PCOS. Personalized weight management strategies – like dietary changes, physical activity, and behavioral support – are essential for achieving these positive outcomes. Moreover, advancements in treatment options, such as GLP-1 medications, offer promising avenues for managing the complexities of PCOS.
In light of these findings, it’s vital for individuals facing PCOS to seek personalized solutions and support systems that fit their unique circumstances. Engaging with healthcare professionals and utilizing comprehensive management strategies can empower women to take control of their health. You’re not alone in this journey; with the right resources and support, meaningful progress in managing PCOS and its associated challenges is possible. Embrace this journey with confidence, knowing that support is available to help you improve your quality of life.
Frequently Asked Questions
What is Polycystic Ovary Syndrome (PCOS)?
Polycystic Ovary Syndrome (PCOS) is a common hormonal condition affecting many women of reproductive age, characterized by irregular menstrual cycles, increased androgen levels, and the presence of polycystic ovaries.
What health complications are associated with PCOS?
PCOS is linked to various health complications, including infertility, metabolic syndrome, a heightened risk of type 2 diabetes, and increased cardiovascular and psychological health risks.
What causes PCOS?
The exact cause of PCOS is unclear, but it is believed to arise from a complex mix of genetic factors and environmental influences, with a significant connection to insulin resistance.
How does insulin resistance affect women with PCOS?
Insulin resistance can lead to weight gain and obesity, making it challenging for individuals to manage their body size, which is crucial for improving health outcomes in those with PCOS.
Can losing weight help with PCOS symptoms?
Weight management is important for improving overall health outcomes in women with PCOS, but it is not guaranteed that losing weight will make PCOS go away.
What are the current guidelines for managing PCOS?
Current guidelines emphasize early diagnosis and tailored treatment strategies that address not only the reproductive aspects of PCOS but also its metabolic and psychological effects.
What innovative treatment options are available for PCOS?
Research is focusing on personalized care and innovative treatment options, such as GLP-1 medications, to help manage the challenges associated with PCOS.
How can individuals manage PCOS effectively?
With the right support and understanding, it is possible to manage PCOS effectively and improve quality of life through comprehensive management approaches.
List of Sources
- Define Polycystic Ovary Syndrome (PCOS): Understanding the Condition
- reuters.com (https://reuters.com/business/healthcare-pharmaceuticals/weight-loss-drugs-fill-treatment-gap-women-with-hormone-disorder-pcos-doctors-2025-12-09)
- Why PCOS remains one of the most misunderstood women’s health conditions (https://advisory.com/daily-briefing/2025/10/21/pcos)
- Polycystic ovary syndrome in 2025—insights and innovations (https://fertstert.org/article/S0015-0282(25)01922-3/fulltext)
- New findings offer fertility hope for women with PCOS | NUHS+ (https://nuhsplus.edu.sg/article/new-findings-offer-fertility-hope-for-women-with-pcos)
- mountsinai.org (https://mountsinai.org/about/newsroom/2025/mount-sinai-duke-university-study-identifies-dna-variants-that-increase-testosterone-production-in-pcos-patients)
- Explore the Connection Between PCOS and Weight Management
- reuters.com (https://reuters.com/business/healthcare-pharmaceuticals/weight-loss-drugs-fill-treatment-gap-women-with-hormone-disorder-pcos-doctors-2025-12-09)
- Tirzepatide Demonstrates Real-World Effectiveness in PCOS (https://clinicaladvisor.com/news/tirzepatide-demonstrates-real-world-effectiveness-in-pcos)
- Weight loss drugs could be a gamechanger for women with a common hormonal disorder (https://cnbc.com/2025/07/20/weight-loss-drugs-could-help-treat-pcos.html)
- The Medical Minute: Irregular periods, weight gain and facial hair? It could be PCOS (https://pennstatehealthnews.org/2025/06/the-medical-minute-irregular-periods-weight-gain-and-facial-hair-it-could-be-pcos)
- Tirzepatide, digital engagement improve weight loss for most women with PCOS (https://healio.com/news/endocrinology/20251110/tirzepatide-digital-engagement-improve-weight-loss-for-most-women-with-pcos)
- Identify Effective Weight Loss Strategies for Managing PCOS
- Weight Management Strategies to Reduce Metabolic Morbidity in Women With Polycystic Ovary Syndrome – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11882674)
- Weight loss drugs could be a gamechanger for women with a common hormonal disorder (https://cnbc.com/2025/07/20/weight-loss-drugs-could-help-treat-pcos.html)
- Revolutionizing PCOS Treatment: How Weight Loss Drugs Are Changing Womens Lives | El Paso Emergency Room (https://eper.com/blog/revolutionizing-pcos-treatment-how-weight-loss-drugs-are-changing-womens-lives)
- phc.ox.ac.uk (https://phc.ox.ac.uk/blog/polycystic-ovary-syndrome-losing-weight-can-help-but-many-sufferers-are-vulnerable-to-bad-advice-on-social-media)
- reuters.com (https://reuters.com/business/healthcare-pharmaceuticals/weight-loss-drugs-fill-treatment-gap-women-with-hormone-disorder-pcos-doctors-2025-12-09)
- Emphasize the Need for Personalized Weight Loss Solutions in PCOS
- reuters.com (https://reuters.com/business/healthcare-pharmaceuticals/weight-loss-drugs-fill-treatment-gap-women-with-hormone-disorder-pcos-doctors-2025-12-09)
- Tirzepatide Demonstrates Real-World Effectiveness in PCOS (https://clinicaladvisor.com/news/tirzepatide-demonstrates-real-world-effectiveness-in-pcos)
- Weight loss drugs could be a gamechanger for women with a common hormonal disorder (https://cnbc.com/2025/07/20/weight-loss-drugs-could-help-treat-pcos.html)
- Revolutionizing PCOS Treatment: How Weight Loss Drugs Are Changing Womens Lives | El Paso Emergency Room (https://eper.com/blog/revolutionizing-pcos-treatment-how-weight-loss-drugs-are-changing-womens-lives)
- Tirzepatide, digital engagement improve weight loss for most women with PCOS (https://healio.com/news/endocrinology/20251110/tirzepatide-digital-engagement-improve-weight-loss-for-most-women-with-pcos)



